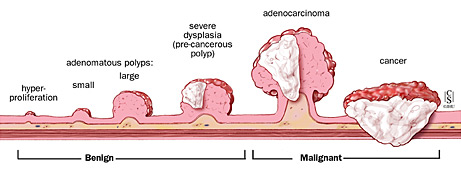
In a landmark study published in 2003, Torlakovic et al. Historically, colorectal polyps were classified as conventional adenomas (adenomatous polyps) and hyperplastic (metaplastic) polyps, with only the former being recognised as having a risk of malignant transformation. This risk in turn informs colonoscopic surveillance intervals. This study has uncovered a potential role for the use of additional serial sections in the morphological reappraisal of small hyperplastic polyps, especially when proximally located.Īlthough serrated polyps have in common a saw-tooth morphology of crypts, it is important to distinguish between hyperplastic polyps (HPs) and sessile serrated lesions (SSLs) because of the inherent difference in risk of malignant transformation. Histopathological distinction between hyperplastic polyps and sessile serrated lesions remains a challenge. An average of 3.6 serial sections were required for a change in diagnosis. They were all less than 5 mm and represented 14.3% of proximal polyps and 10.4% of distal polyps. After 8 additional serial sections, 11 (10.7%) were reclassified as sessile serrated lesions. Of the 103 confirmed hyperplastic polyps, 7 (6.8%) were proximal, and 8 (7.8%) had a largest fragment size of ≥5 mm and < 10 mm. Of an initial 147 hyperplastic polyps from 93 patients, 9 (6.1%) were classified as sessile serrated lesions, 103 as hyperplastic polyps, and 35 as other. Eight additional serial sections were performed for the confirmed hyperplastic polyp group and reviewed. The slides were reviewed and classified as hyperplastic polyps, sessile serrated lesion, or other, using current World Health Organization criteria. MethodsĬlinicopathological data for all colorectal hyperplastic polyps diagnosed in 20 was collected. Our aim was to reclassify previously diagnosed hyperplastic polyps as sessile serrated lesions or confirmed hyperplastic polyps, using additional serial sections. Sessile serrated lesions and hyperplastic polyps are types of serrated polyps which confer different malignancy risks, and surveillance intervals, and are sometimes difficult to discriminate. However, if larger polyps or cancerous polyps are found, you may need several follow-up colonoscopies in the span of a few years.The histological discrimination of hyperplastic polyps from sessile serrated lesions can be difficult. If small polyps are found, your doctor may suggest a return visit in as little as five years. If your doctor doesn’t find any adenomas or polyps, the next screening may not be necessary for 10 years. Ask when you should be screened again.You can also reduce your risk for polyps and cancer by losing weight and exercising. While it’s unclear why colon polyps develop, doctors do know you can lower your risk by eating a healthy diet with fiber and reduced fat. 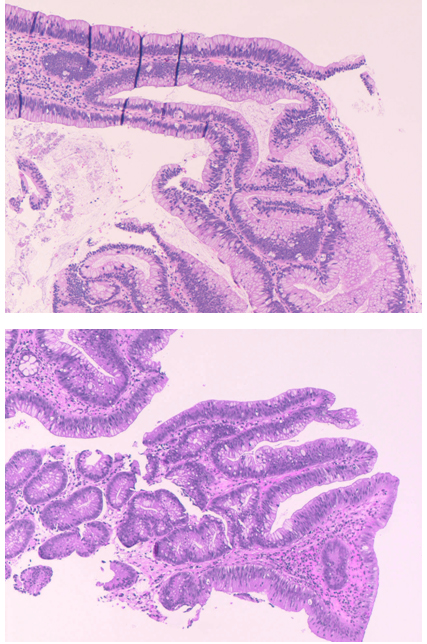
If the polyp is precancerous or cancerous, your doctor may want to remove it quickly. This may include a watchful waiting period where you don’t take action. If polyps were found and tested, what needs to happen to them? Talk with your doctor about a treatment plan. They’ll likely have images of any polyps, and they’ll also have results of biopsies back within a few days. In your follow-up appointment, ask your doctor about the results of the colonoscopy. Your doctor can talk about your individual risk and things you can do to lower your risk in the future. Lifestyle and genetic factors may influence your risk for developing colon cancer or precancer. Ask if you’re at an increased risk of colon cancer.Use these talking points to start the conversation: If you’re preparing for a colonoscopy or colon cancer screening, talk with your doctor about your risk for colon cancer and what will be done if polyps are found.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
